LIVERPOOL- Experts at Cop28 this month are advocating for a groundbreaking initiative to electrify all healthcare facilities in low-income countries using solar energy within five years, at a cost estimated to be less than $5 billion. The proposal aims to eradicate the life-threatening risks posed by power outages in medical settings, particularly affecting vulnerable populations.
Salvatore Vinci, an adviser on sustainable energy at the World Health Organization (WHO) and a member of its Cop28 delegation, emphasized the urgency of the initiative, stating, “I would like the international community to commit to a deadline and funding to electrify all healthcare facilities. We have solutions now that were not available 10 years ago – there is no reason why babies should be dying today because there is not electricity to power their incubators. It’s a low-hanging fruit. There is nothing stopping us.”
Approximately 1 billion people worldwide lack access to healthcare facilities with stable electricity connections, including 433 million in low-income countries relying on facilities with no electricity, according to the WHO’s Energising Health report published in January.
Electricity is fundamental for healthcare facilities, powering crucial devices like ventilators and cardiac monitors, as well as providing basic amenities such as lighting. The absence of these essentials can escalate routine conditions into deadly situations. Extreme weather events, common in countries vulnerable to their impact, often result in power outages.
Hippolite Amadi, bioengineering professor at Imperial College London, highlighted the dire consequences, stating, “We don’t know how many people die each year because of power outages. Nobody puts ‘power outage’ as a cause of death on a death certificate. As we speak, patients in low- and middle-income countries are dying due to power outages and poor lighting.”
Maternal and surgery patients face immediate risks due to the lack of lighting, while an unreliable energy source hinders long-term treatments such as kidney dialysis. The burden of chronic non-communicable diseases (NCDs) is rising in the global south, adding strain to poorly electrified facilities.
In Central African Republic, where citizens are most likely to die prematurely from an NCD, over 60% of healthcare facilities report having no access to electricity.
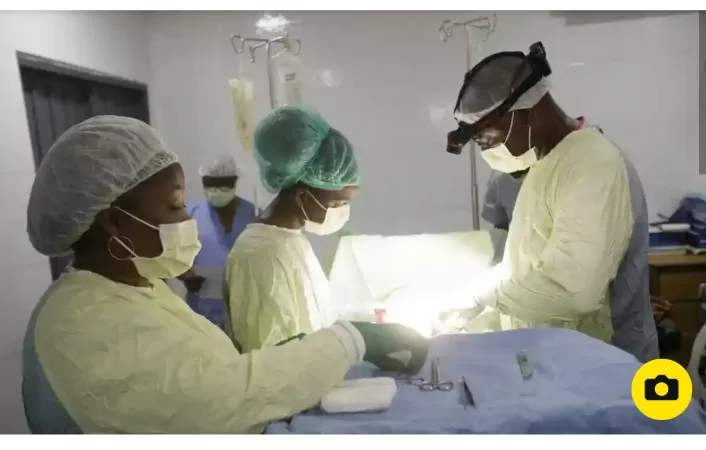
Emmanuel Makasa, an orthopedic surgeon in Zambia, emphasized the impact of inadequate lighting on medical professionals, stating, “The best surgeon in the world cannot do good work if he cannot see what he is doing. You would never ask a tailor to work in the dark, why would you expect it from a doctor?”
Despite the challenges, success stories like electrifying maternal healthcare centers in Nigeria’s Niger state showcase the potential of solar solutions. Vinci pointed out the decreasing costs of photovoltaic modules and batteries, making cost-effective and reliable solar energy systems viable for rapid deployment.
“We can go and deploy a cost-effective and reliable solar energy system at a facility in a matter of a few days. We don’t need to wait any more,” Vinci emphasized.